A Silent Struggle: The challenge of embracing hearing instruments in mild hearing loss cases
In his regular From the Oval Window column for Audio Infos UK magazine, audiologist Rául García-Medina looks at resistance to hearing aids in mild hearing loss patients, considering among other factors, the prevalence of anosognosia.
There is a new EuroTrak studyby EHIMA (Anovum) for the UK, for all to scrutinise and benefit from the insight it provides.
I have been following these consumer studies for quite some time now, firstly with the inception of MarkeTrak in the US, and later the EuroTrak surveys. The first MarkeTrak survey – the OG in its field – appeared in 1989. Its European counterpart appeared some 20 years later, in 2009, with studies from the UK, Germany, and France. Other European and non-European surveys followed.
MarkeTrak 2022 and EuroTrak 2022 UK have some similarities in their findings. Regrettably, and like most of you, I only have access to publicly available articles that include highlights from each MarkeTrak report, and I am thankful for a glimpse of the latest publication, to Thomas A. Powers, PhD, and Kate Carr for their article in The Hearing Review MarkeTrak 2022: Navigating the Changing Landscape of Hearing Healthcare. The Hearing Industries Association (HIA) is the organisation that commissions the detailed survey with comprehensive findings. Unfortunately, the full reports are confidential to their members.

Why am I seeing increasing mild HL cases?
As always, there is much to analyse and interpret, and different enquiry angles provide different insights. For a long while now, and possibly more of late, I am seeing a growing number of mild hearing loss cases. Perhaps this results from increased public focus on hearing healthcare research and general awareness on hearing loss comorbidities. One reference often quoted by patients is the 2017 Lancet Commission on dementia prevention, intervention, and care, as well as the follow-up 2020 report from the same publication. It would appear that these publications and the general media interest they attract have reached our patients, more of whom venture out to our clinics to see if their hearing health is as it should be, even if the perceived difficulties are mild.
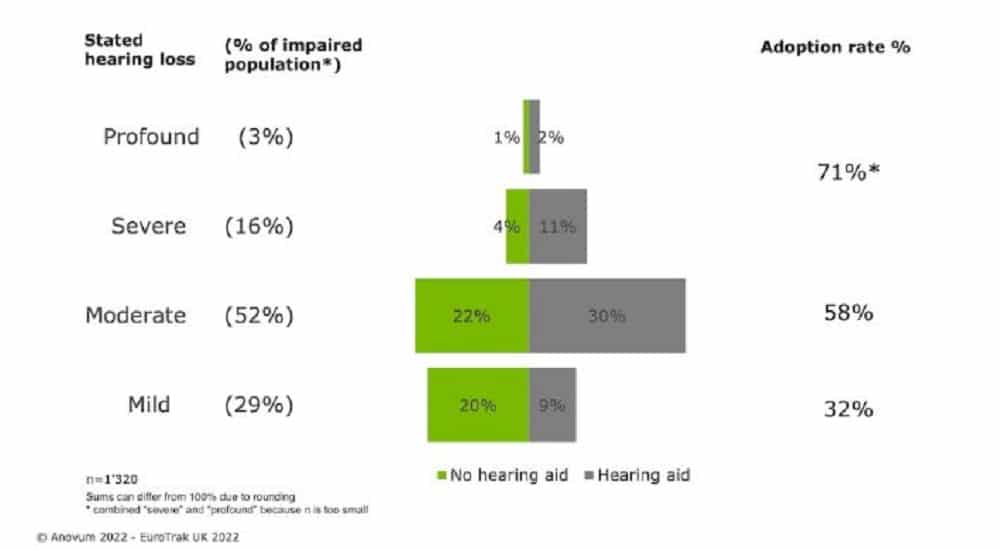
This segment of the hearing impairment population has always posed greater challenges for the hearing healthcare professional. The EuroTrak 2022 UK survey highlights that 29% of the hearing-impaired population self-reports mild hearing loss. Linked to that figure is a low 32% adoption rate. In comparison with the same data from the 2018 publication, 30% of the hearing-impaired population self-reported mild hearing loss, and the adoption rate then was also a mere 30%. So, no changes here really. But it is true that adoption rates revealed in the 2015 and 2012 studies were then worse: an appalling 18% and 13% respectively, although self-reported mild hearing loss percentages amongst the hearing-impaired population were consistent with later figures, at 30% and 29% respectively.

RGM Audiologist Raúl García-Medina: “Perhaps the profession is still not creating the right education and awareness campaigns.”
So why is it that this segment of the hearing-impaired population remains adamantly resistant to embracing hearing instruments?
I think you will all draw your own conclusions, and they are probably all valid. But perhaps the profession is still not creating the right education and awareness campaigns, such as those that have so far proved so fruitful when disseminating information about the correlations between hearing loss and cognition.
The January 2023 Hearing Review articleby Dr. Douglas L. Beck Cognition and Audition: Perspectives and Review 2023 raises very interesting questions that its author hopes we will find answers to in the next few years. There are some key ones that may relate well to the mild hearing-impaired population and the conundrum around their very low adoption rates.
1. How much (if any) cognitive benefit might one expect from hearing aid fittings?
2. Who are the best candidates regarding type and degree of hearing loss?
3. What about OTCs versus prescription aids – same or different cognitive benefits?
Certainly, if we find the answers to the above questions we will be able to build a more robust empirical evidence base for relating to our patients. Assuming that the answer to the tough question 1. is indeed some degree of benefit, and that the answer to question 2. includes mild hearing loss cases, and if there is a cheaper version of prescription aids available, there will be few arguments the mild hearing-impaired cohort can use to refute a treatment recommendation.
Dr. Beck also points out that this self-reported mild hearing loss could also be non-auditory related, which adds weight to the now old adage that we need to improve our understanding and positioning within the healthcare sector in relation to cognition and the brain. You simply cannot afford to dismiss these cases with a simple PTA anymore.

To add to the above, EuroTrak 2022 UK also states that there are potential social cost-savings due to the use of hearing instruments: improved work competitiveness, lower risk of depression, less fatigue in the evenings, and improved quality of sleep. Furthermore, we could be helping our patients for many years to come, particularly if the mild cases attend our clinics when they are relatively young. EuroTrak reports that the average renewal time of the hearing instruments is around every 4 years. This same renewal period was reported in the 2018 EuroTrak UK study.

The general non-adherence of the mild hearing-impaired segment to embrace our treatment recommendations along the aforementioned lines is surely multifaceted. The reasons are often driven by social determinants of health, but others are intrinsic. The term anosognosia was referred to recently in another of Gus Mueller’s regular interview articles in AudiologyOnline, entitled 20Q: Audiology – There’s an Art to this Science, this time with Barnaby Growling (pseudonym – read it to find out). Anosognosia is a condition in which an individual is unaware or denies the existence of a physical or mental impairment, despite evidence to the contrary. In the context of hearing loss, the condition relates to the phenomenon whereby an individual with hearing loss is unaware of their condition or denies the existence of their hearing loss. Most of the non-adherence is intentional, and the patient bases it on experience, belief systems, and most certainly knowledge. These patients with mild hearing loss may not understand why they need a certain treatment. What is crucial in dealing with them is to create a good rapport and build reciprocal trust. Getting to know the patient is of utmost importance in order to arrive at the right Socratic questions to find out why they have attended your clinic but are not taking up your treatment recommendations.
Some ways to tackle non-adherence
It is also true that there is no one-size-fits-all approach to achieving greater adherence or uptake of the treatment recommendation, but some methods may increase success. Approaching the patient with a positive is a must. For example, ask: “what can we do together to make this work? Or, what are you questions about this particular treatment recommendation? Then try to focus on the positive things that you can act upon, and create a blame-free culture instead of leaving the patient with a negative feeling or the concern that you do not agree with their reasoning or choices. Ultimately, the goal is to provide good care and treatment.
The most important thing is to be honest and very transparent with the patients you feel are not making the appropriate strides forward. Perhaps even recommend further investigation, or refer on to another clinician for a second opinion if your own audiological or other resources are limited. Or even improve your own knowledge and understanding of the current trends in our profession, and equip your clinics to be able to deal with these cases. What is becoming clearer from research and investigations is that we are often sending individuals with self-perceived mild hearing impairments away when in reality, they are trusting you to evaluate their listening skills, and a simple PTA is not going to get to the meat of the problem. I hear you Dr. Beck, you have been saying this for a while: “listening is where hearing meets the brain”. The future of Audiology seems also to be in the brain.
References:
Anovum – EuroTrak UK/2022/
Powers TA, Carr K. MarkeTrak 2022: Navigating the changing landscape of hearing healthcare. Hearing Review. 2022;29(5):12-17.
Source: Audio Infos UK issue 152 January-February 2023
 Sign in
Sign in


